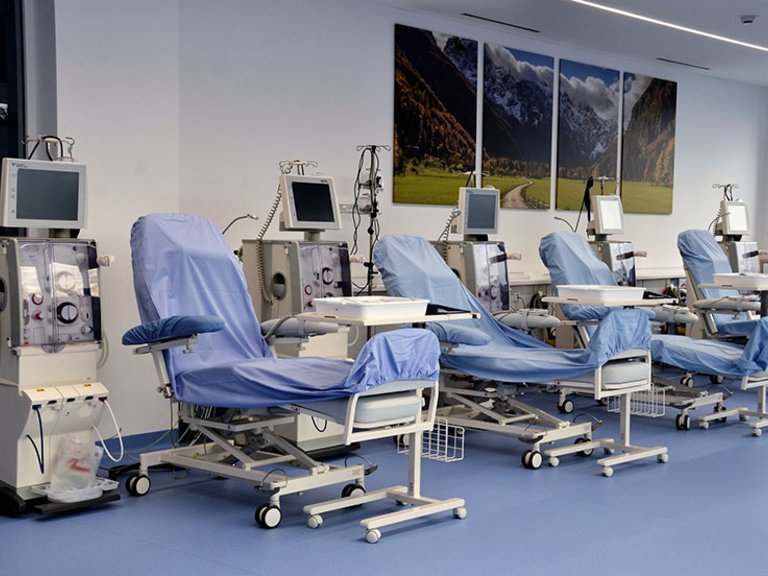
Shared and self-Care of patients in a dialysis center represents the equivalent level of independency in the treatment as home haemodialysis. The key to shared and self-Care is the involvement of the patient into the treatment at most or all steps.
Shared care is an important part of how we operate. We believe that for some, shared care actively encourages and empowers patients in the participation of their treatment building confidence in meeting their individual health care needs. Our shared care approach is built on reflecting the needs and preferences of patients, their families and carers. To offer patients choice and feel they have autonomy within their own care our nurses are highly trained to support patients who opt for a shared care approach to their treatment.